What is a Pediatric Dentist (Pediatric Dental Specialist)?
During six years of higher education, students take 30 classes and 15 basic laboratory classes in pediatric dentistry and undergo two weeks of clinical training in dentistry in a year. This cannot be considered very substantial. After graduating from the university, they are obliged to work as dental interns for a year, during which they mainly learn the fundamentals of clinical dentistry for adults. To be a pediatric dental specialist, they are required to work at a training facility specifically for pediatric dentistry for five years after residency training and then pass the test to become a specialist in pediatric dentistry.
New dentists who enter into the pediatric dental laboratory after one-year post-graduation training can hardly treat a child's toothache. Therefore, dentists in general practice who have studied general dentistry have a limited knowledge of and expertise in dental care techniques for children. It is not surprising that there are a lot of patients who say, "I took my child to a dental clinic, but the dentist wouldn't even bother with treatment and only introduced me to a pediatric dentist."
As shown in Table 1, out of 4,300 members of the Japanese Society of Pediatric Dentistry, these pediatric dental specialists number about 1,600, and they are heavily outnumbered by 15,000 pediatricians.
Table 1. Number of members of Japanese Society of Pediatric Dentistry (2008)
| Kita Nihon Branch | 597 |
|---|---|
| Kanto Branch | 1,674 |
| Chubu Branch | 536 |
| Kinki Branch | 553 |
| Chu-Shikoku Branch | 426 |
| Kyushu Branch | 554 |
| Total number of members | 4,340 |
| 1,550 of the members are pediatric dental specialists | |
Pediatric Dental Care System (What is the difference from other health care systems?)
Routine medical checkups are a feature of the unique system of pediatric dentistry. The inside of the child's mouth changes with age, from birth to the primary dentition period (2 to 6 years old), mixed dentition period (6 to 12 years old) when both primary and permanent teeth exist and the permanent dentition period (12 years old and after). According to the changes, as the site of predilection for caries moves, the method of prevention also changes. In addition, problems tend to occur when children cut new teeth. For these reasons, routine checkups are recommended. This system applies to all child patients. So, unlike the general dentist where visits and treatments end when the particular teeth have been treated, it is not an uncommon for patients to continue to have routine checkups until they become at least fifteen or sixteen years old, or twenty depending on the patient.
Patients have the routine checkups once every four or five months. In no other specialty do doctors maintain such a long-term relationship not only with patients but also with their families. We have heard of a pediatric dentist who was invited to the wedding of a former child patient. This system enables us to gain a deeper understanding of children and their families.
Treatment of Children's Teeth
1. Achieving rapport
It is not too much to say that medical care starts by achieving rapport. Treatment of a child's caries starts by having the child sit in the chair alone, injecting local anesthetic into the gum and drilling the tooth. It is not over easily just because the patient is only a child. Each visit entails enduring 30 dreadful minutes of treatment. During that time, how smoothly treatment is carried out depends on the degree of trust that child places in us. We have to welcome the children by opening our hearts so that children from two- to three-year-old to fourteen- to fifteen-year-old will open their mouths widely for us.
How does rapport develop? It is born out of conflict between children and adults. Though it is easy for adults to bring children into submission by force, we refrain from that even for the sake of treatment. As dentists, we provide dental treatment of a certain standard and also assume a certain level of understanding in the patient, which is above what we can naturally expect of children. In other words, there is some distance between where they are and the treatment. We go down to their level and then bring them up to the treatment line little by little. We get them ready to receive treatment through small and regular steps that familiarize them without using force or hurting their pride. When they are finally ready, the treatment begins.
For children, the thirty-minute treatment period is a peculiar experience that they do not encounter in daily life. They experience fear, discomfort, noise, and stress, including pain. As doctors, we go forward little by little, imagining the mind of children at the limit of their tolerance levels. In this way, the mental defenses they put up against us begin to come down. Before long, we feel them becoming less tense and their bodies relaxing. Then they return to their natural selves, they have a confident look in their eyes or a sense of security that comes from having successfully cleared the inexperienced zone. Their trust in us is born out of this conflicted feeling. This sort of deeply felt experience that touches their heart is one that will stay with them.
Mothers and fathers also sense this as they watch us struggle nearby . Some fathers go back home with emotion, saying that they feel as if they had seen an unexpected side of their children. This trust that both children and parents place in us helps us provide better treatment in the future.
2. Systematic Desensitization (Tell, Show, Do)
Systematic desensitization is one of the methods we use to help children adjust to the treatment. The clinic is full of metallic sounds, and everything is pointed and shiny, and new for children to see and touch. We have the children pick and touch them, starting with the most basic one. Our explanation likens them to familiar things. To use a textbook-like expression, this is called systematic desensitization (Tell, Show, Do). "This is a cleaner which sucks up saliva or food particles in the mouth, and this is a mechanical toothbrush." We put a brush on the tip of a drill to rotate in front of their face, take it to their mouth and brush their teeth. We spurt water and suction it with cleaner. In the course of repeating these actions, even children who refuse to listen become cooperative patients before you know it. Child patients who were full of fear lose it completely when they know the truth. Unlike real adults who suspect that it is really going hurt, children are not suspicious. This is why we can't lie.
Another method is called modeling. In the modeling method, the child patient is shown the actual treatment of another child or a video and told, "Everybody does it, so you can, too!" However, this does not always work well, because there are many children who lose confidence more when seeing a child who is doing well. So, we use this model to tell the child, "You are a good boy (or a girl) because you're not screaming like that other child next to you." Then the child responds, "Yes, I am!"
3. Children of All Types
In most cases, however, these models do not reflect reality. Take a three-year-old child who visits our clinic with four or five bad teeth. The child, who has been in day-care since infancy calmly comes into our office, sits in the chair with great interest and starts to play with the water in the cup. Treating such a patient child is easy. The mother also enjoys her time beside us text-messaging on her cell-phone, saying "I'll leave it up to you." We sense a distance between the mother and the child.
On the other hand, there is the child who grips the parent's hand, ready to burst into tears at any moment. A soft tap on the back and gentle push toward the chair is enough to cause crying as if the child had been stung by bee. Of course, the parents are nervous, too. Dental treatment is still a long way off. The more the relationship between parents and the child is filled with love, the more difficult it is for a third party to come between them. Of course, we know that those children are actually very good, calm and obedient.
Our first meetings with children are all very different.
4. Treatment of Uncooperative Children
Dental treatment does not end with just taking a temperature, having a look at the patient's throat, applying a stethoscope to the chest and saying, "You have caught a cold." The child patient has to endure the fearful thirty minutes. Despite extensive and painful caries, which cannot be left untreated, the child is refusing treatment. We manage to give emergency treatment and have the patient make repeated visits to practice, but the child never reaches the treatment line.
For children who refuse treatment in a determined manner, we have two choices: either compulsory treatment or intravenous sedation (general anesthesia). Compulsory treatment entails strapping the patient down to the bed with a net or a bath towel. The patient's fear reaches a peak when the treatment starts and they resist violently.
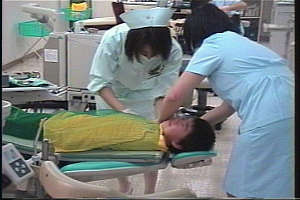
However, as they come to know that it doesn't hurt to be given an injection after surface anesthesia and that drilling a tooth is not major surgery, they calm down.
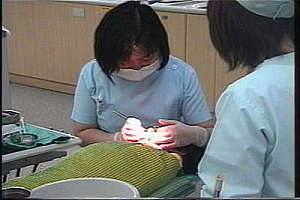
When we see that they have come to accept the treatment, we slowly begin to unstrap the net. By the end of the treatment, the net is completely unstrapped.
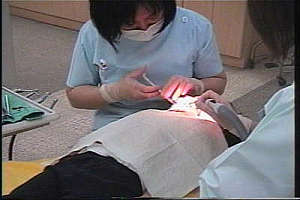
The children then come to realize that they no longer need the net during treatment. If the patient has an ailment that cannot be left untreated, this temporary compulsory treatment is given after the parents receive a full explanation and give their consent. Few parents select intravenous sedation or general anesthesia unless the child is handicapped.
5. Treatment of a handicapped children
When a patient with extensive caries cannot fully understand the treatment, we use general anesthesia. When a child clearly has a mental handicap and has been diagnosed as such, we are able to properly respond from the first. But, in the case of children with undiagnosed developmental disabilities, such as ADHD or Asperger syndrome, it takes some time and effort before we are able to know the right method for the child. On the first impression, the perception that "this child is a little different," may be utilized for this early diagnosis of developmental disabilities.
An adult who is diagnosed as having Asperger syndrome once told me, "I was diagnosed with Asperger syndrome when I was in the third grade of elementary school. Until then, I was excluded by my classmates and even disliked by the homeroom teacher. After I was diagnosed, however, the attitude of the people around me suddenly changed and the teacher also became nice to me. I think the homeroom teacher heard about my diagnosis from my mother, and feeling bad about how he had treated me, told my classmates. I wish I had been diagnosed earlier."
This was a startling story for us who sometimes provide dental treatment to similar children. We should try not to be like the homeroom teacher. At the same time, I was worried that I might have treated children like the homeroom teacher without knowing it until then.
Prevention of Caries
1. Streptococcus mutans is transmitted from mother
About 300 kinds of bacteria live in the mouth. About 30 percent of them are streptococcus, and among them, Streptococcus mutans resolve sugar, resynthesize polysaccharide and produce acid, which is a powerful enemy of the teeth. Where does this mutans come from? It is mainly transmitted by the mother when licking the rubber nipple of baby bottle to check the temperature of the milk, feeding milk from mouth to mouth or by spoon, or kissing. Therefore, at the time of prenatal checkup, all mothers-to-be have to clean their own mouths first. It is well known that the number of mutans detected in saliva is proportional to that of caries in the mouth. Prevention of tooth decay starts before the child is born.
2. Dietary habits are the basis of lifestyle.
Sugar in the mouth decreases the mouth's pH to acid. Enamel begins to demineralize when pH comes down to 5.4 and below. Then, saliva with high pH begins to appear and the value goes back to normal in about 20 to 30 minutes. Thus enamel which once begins to demineralize would be remineralized soon. However, if you snack on a bag of sweets for half a day, the pH value in the mouth continues to decrease, advancing demineralization and causing a cavity in due course.
Most children stay close to their mothers until they reach the age of three. According to some reports, it is good for child development when the child's life is not solely dependent on the mother, but a responsible third party is also allowed to look after a part of the child's life. In case of young children, the lifestyle of mother has a huge and direct effect on the production of caries in children. As life revolves around food and snacks, we always check dietary habits during routine checkups from the point of view of oral health. When patients answer that their lifestyle is "normal," the word "normal" is problematic, and some realize how abnormal their "normal" dietary habits are.
3. Is extensive caries neglect?
Children with extensive caries tend to have parents or guardians with problematic dietary habits. They often have no interest in the oral health of children and some of them do not brush their children's teeth and even do not (or cannot) visit the dentist. Caries is not trouble that everybody has to experience. If children have only one or two decayed teeth, that is OK, but some of them visit us with many decayed teeth. In that case, we take the extra step of asking parents about their home lives. Why do the children have a lot of decayed teeth? Our support for children efficiently prevents teeth from decaying, regains the rhythm of life by changing snacking habits and lends an ear to mothers who are tired of child rearing. We also introduce the activities of community centers in their area.
When children visit us in dirty clothes, we check whether they have injuries on their bodies or not. Out of new patients we have seen for 10 years, about 15 % of their chief complaints are external injury of teeth. In case of external injury, we check whether the location or cause of the injury is unnatural. When in doubt, we report to the municipal office or healthcare center without further delay. We are often told that they already had an eye on the said child. There also are some cases that cannot be detected if the work of pediatric dentistry is limited to a tooth repair. When this happens, we keenly feel the responsibility of working with children.
Pediatric Dentistry and Child Science
Various specialists working with children devote themselves to pursuing expertise in their own specialized areas. For this reason, specialists tend to be unconcerned with areas other than their own specialty and to leave those things to other specialists. This results in various problematic cases. For example, an enthusiastic elementary school teacher sees a developmentally-disabled child as a problem child. A patient complains that the medical staff cured him physically but inflicted lasting psychological pain. A child ended up with many cavities after following a pediatric doctor's advice to drink sports drinks to prevent dehydration. With nurses and hygienists do not understand how children feel, we can almost hear children crying, "What's going on!" Moreover, other problems are arising in children's food, play, toys, cell-phones, internet, etc. There's no problem if parental guardians can protect and foster children with sound judgment in a home that is their foundation, but nowadays it is pointed out that there are problems in that very home.
The lives of children will not improve without the collaboration of specialists from each field of education, medical treatment, healthcare and welfare. From that point of view, the pediatric dentist regularly observes children during a certain period and specializes in the oral diseases that noticeably reflect their lifestyles, and it is our duty not only to look inside their small mouths but also to apply our expertise to support child rearing in general. I think this is the role of pediatric dentistry as an area of Child Science.
References
- Watanabe S., Hiraiwa M. Yasashiku Manaberu Kodomono Ha (Easily Learning Children's Teeth) Shindan To Chiryo Sha, Tokyo 2008
- Watanabe S. Issues of Pediatric Dentistry for 21st Century, Toward the establishment of Japan Kosodate Gakkai, Pediatric Dental Clinic 8:44-45, 2003
Reprinted from Child Science vol.5, published by Japanese Society of Child Science














